
New Healthcare Consumer Insights Survey Reveals How Members Perceive Their Commercial, Medicare and Medicaid Plans
Carenet has published its latest consumer health report and uncovered opportunities for insurance plans to improve the member experience. Based on a third-party survey of more than 1,200 adult respondents in the United States who have health insurance, the report provides an in-depth overview on how members really feel about their insurance plans.
The report, Healthcare Consumer Insights: Understanding the Health Insurance Member Experience, reveals members’ perceptions and validates their demand for improved experiences.
As healthcare costs continue to rise and consumers have increasing options for managing their care, our findings provide an in-depth overview of how members view their commercial, Medicare, and Medicaid plans.
DOWNLOAD THE FULL REPORT HERE.
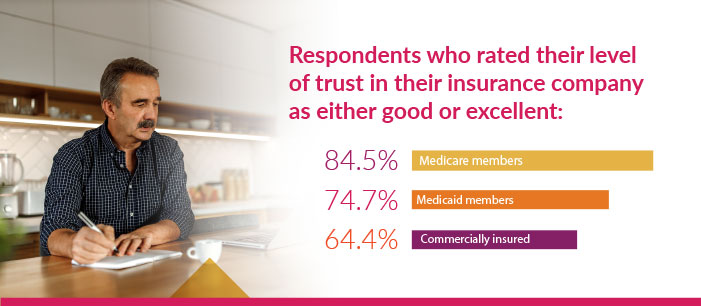
Medicare and Medicaid Members Have Higher Levels of Trust
When indicating their level of trust in their insurance company, most Medicare and Medicaid members gave a rating of either good or excellent. In comparison, a lower percentage of commercially insured respondents gave high ratings on the question of trust. These findings challenge the assumption that the commercial insurance consumer experience is inherently superior to Medicare and Medicaid.
Learn more about Carenet’s engagement solutions that help health plans serve the complex Medicare and Medicaid populations.
Language Barriers and Other Phone Support Pain Points
More than a third of respondents indicated that a conversation with their health insurer was hampered by a language barrier. As the number of Americans who speak a language other than English in their home has more than tripled since 1980, it’s critical that health insurance phone support includes multi-language capabilities to provide equitable customer service to all members.
Furthermore, an overwhelming majority of respondents (89.1%) want phone representatives who are well-versed in healthcare. Among those who ranked health insurance companies unfavorably for phone support, nearly half said the representative did not understand their issue.

Health insurance phone support must include multi-language capabilities to provide equitable customer service to all members.
Consumers Want Online Tools and Apps
Among those who indicated that the use of technology was either very or somewhat important when managing one’s health, responses were similar across insurance types and age groups.

This emphasizes how consumers are accustomed to using online tools and apps in many daily transactions such as retail purchases, banking, and ridesharing. They want access to the same conveniences when managing their healthcare.
The popularity of technology use across respondents points to the need for serving plan members with a balanced combination of human and digital interactions.
Carenet is using the findings of the Healthcare Consumer Insights: Understanding the Health Insurance Member Experience survey to elevate our exceptional payer solutions that simplify and modernize the health plan member experience.


